A VPN (Virtual Private Network) is not explicitly required by HIPAA regulations, but many healthcare organizations use VPNs as part of their security strategy to become HIPAA compliant. The HIPAA Security Rule requires appropriate protections for electronic protected health information without mandating particular technologies. VPNs help meet these requirements by encrypting data transmission, establishing secure remote access, and creating access controls that protect patient information from unauthorized disclosure.
HIPAA Network Protection Standards
The HIPAA Security Rule sets standards for protecting electronic health information without prescribing exact technical implementations. Healthcare organizations must implement safeguards that protect data integrity, confidentiality, and availability. Network protection measures matter when transmitting patient information across public networks. To become HIPAA Compliant, organizations must verify that transmitted information remains unaltered during transfer. Only authorized personnel should view sensitive data, regardless of whether access occurs within healthcare facilities or from remote locations. Many healthcare providers use VPNs to address these requirements, especially for staff working outside main facilities.
VPN Encryption Benefits
VPNs establish encrypted connections between devices and healthcare systems, creating protected pathways for data movement. When staff use public WiFi or home networks, this encryption prevents interception of patient information. Most VPN systems include authentication protocols that confirm user identity before granting system access. Access limitations can be configured to restrict which systems and information each user can view through VPN connections. Healthcare organizations often include VPN implementation details in their documentation during compliance audits or assessments, demonstrating how they protect data during transmission.
Securing Off-Site Healthcare Access
Medical professionals increasingly need access to patient records from various locations outside traditional facilities. Remote clinical work, telehealth appointments, and home-based administration all require secure handling of protected health information. Regardless of work location, HIPAA compliance demands consistent data protection standards. VPNs create secure connection tunnels that help maintain this protection across various networks and locations. For remote work to succeed, organizations develop clear guidelines about when VPN use becomes mandatory and how staff should establish secure connections. Mobile device management typically works alongside VPN protocols to ensure all endpoints meet security standards.
Exploring Security Alternatives
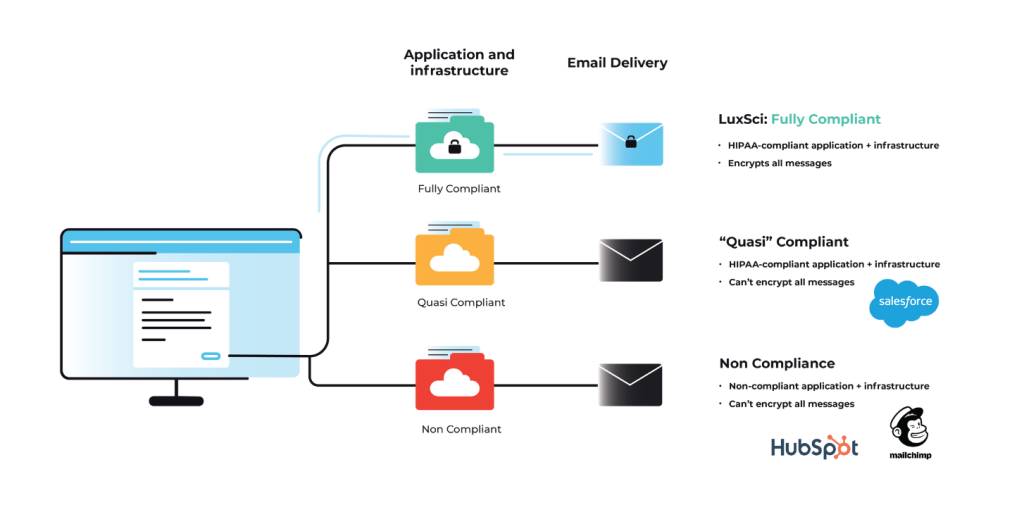
Healthcare organizations can meet HIPAA requirements without VPNs through several alternative approaches. Applications with built-in end-to-end encryption create secure channels for data transfer without full network encryption. Many cloud platforms designed for healthcare include sufficient authentication and security features for certain workflows. Some organizations implement zero trust architectures that verify every access request rather than relying on perimeter security. In practice, many healthcare systems use multiple security technologies rather than depending on any single solution. What matters for HIPAA compliance isn’t the technology chosen, but whether patient information remains properly protected throughout its lifecycle.
Technical VPN Deployment Factors
When implementing VPNs for healthcare environments, several technical elements require attention. Encryption must meet current standards like AES-256 to adequately protect healthcare data. Authentication should involve multiple verification factors beyond passwords alone. Usage monitoring helps identify unusual patterns that might indicate security problems. Staff need training on correct VPN procedures and potential security risks. IT support must address connection difficulties promptly, as frustrated users might otherwise bypass security measures. How these elements work together determines whether VPN deployment strengthens or weakens overall security posture.
Compliance Documentation Practices
HIPAA requires thorough documentation of all security measures and risk evaluations. Security policies should describe VPN usage requirements, configuration standards, and monitoring practices. System architecture documentation must show how VPN connections fit within the overall network design. Regular risk assessment examines potential vulnerabilities in VPN implementations. Response plans outline steps to address potential VPN security incidents. Well-organized documentation helps organizations demonstrate reasonable security efforts during regulatory reviews. During audits or investigations, clear records of security implementation decisions provide evidence of due diligence in protecting patient information