The demand for in-home care is growing as patients increasingly seek personalized, convenient healthcare in the comfort of their homes. A key reason for this increase is the rise in the number of baby boomers, i.e., people aged 65 and older, opting for in-home care.
In fact, as of 2020, there were approximately 76.4 million Baby Boomers in the United States, with projections indicating that by 2040, there will be roughly 80.8 million Americans over the age of 65. Consequently, the need for in-home care services will only grow to accommodate the health needs of this expanding demographic.
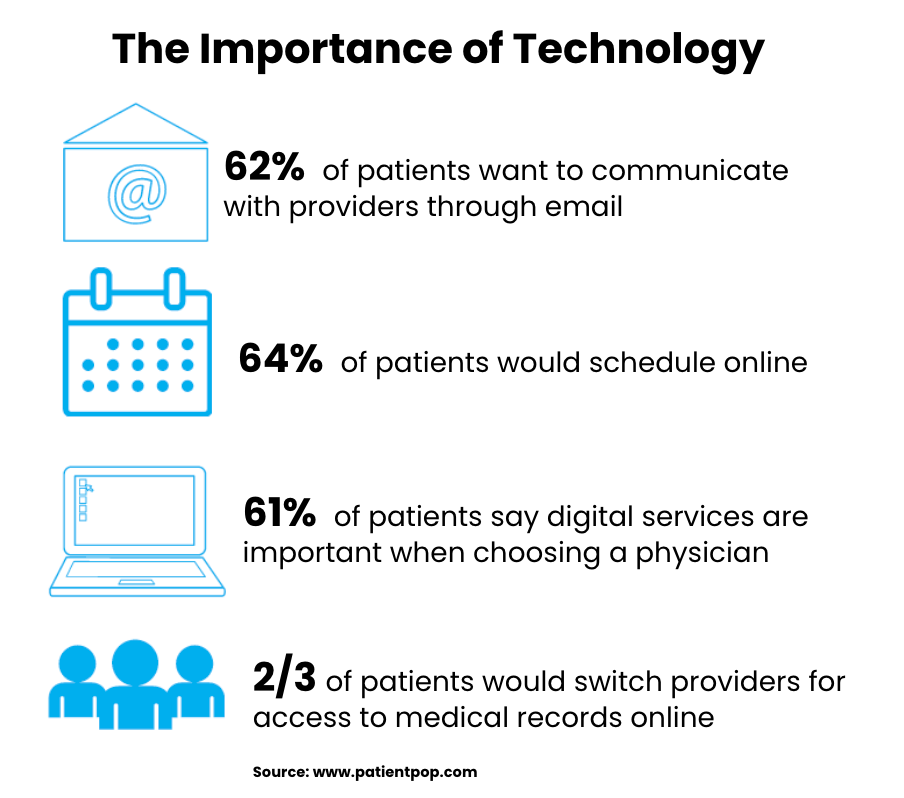
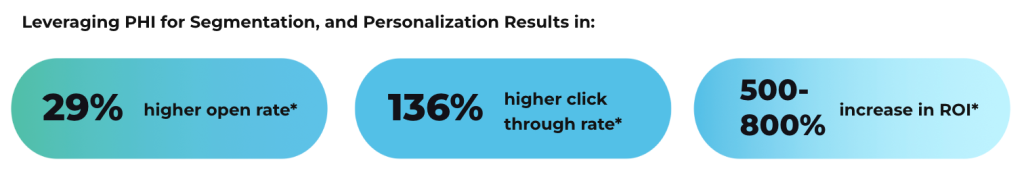
For in-home care providers, remaining competitive in this space requires increased levels of patient engagment over digital channels and the inclusion of protected health information (PHI) to personalize communications. As a result, incorporating secure, HIPAA-compliant email communications and campaigns into your in-home patient outreach efforts both enhances engagement and yields significant operational and financial benefits.
In this post, we explore 7 impactful use cases for HIPAA-compliant secure communications for in-home care, including how providers can harness them to achieve their efficiency goals and growth objectives, while improving health outcomes for patients.
What Are the Benefits of HIPAA-Compliant Email for In-Home Care Providers?
Before we dive into the most common email use cases for in-home care providers, let’s look at why adopting secure, personalized communication strategies offer several advantages:
- Avoiding the Consequences of HIPAA Non-compliance: including sensitive patient data in communications without implementing the security measures required by HIPAA can incur financial (fines, compensation), operational (time spent mitigating security threats), and reputational (being seen as untrustworthy with PHI) consequences.
- Enhanced Efficiency and Outcomes: streamlined communications, such as automated appointment reminders, reduce administrative tasks and missed appointments, allowing staff to spend more of their time engaging patients to drive better health outcomes.
- Improved Patient Satisfaction: timely, relevant, and personalized communications demonstrate a commitment to patient well-being and positive engagements, fostering trust and loyalty.
- Cost Savings: Secure, personalized communications lead to significant cost reductions by preventing miscommunications and the resulting complications.
- Increased brand connection: with HIPAA-compliant communications, you can foster a better understanding of the full extent of your capabilities, the value you provide, and, ultimately, the vital role you play in your patients’ healthcare journey.
High-Impact HIPAA-Compliant Use Cases for In-Home Care
1. Appointment Reminders
Missed appointments are a substantial financial burden on healthcare organizations. In the U.S., they result in an estimated $150 billion in losses annually, with each no-show costing businesses approximately $200 per hour.
Sending personalized, secure appointment reminders via HIPAA-compliant email and text messaging can significantly reduce no-show rates, cutting costs, boosting revenue, and, most importantly, increasing patient adherence to care. Better still, appointment reminders can be automated, e.g., with confirmations sent at the time of booking and reminders scheduled to go out a few days before the appointment. This not only ensures consistent communication, with minimal additional administrative overhead, but also increases the utility and value of the in-home care service.
2. Follow-Up Communications
Frequent follow-up email communications are an effective way to monitor a patient’s progress, ensuring adherence to treatment plans and enabling them to adapt a health regime according to potential changes in their condition.
A few examples of situations that warrant a follow-up email include:
- After an initial consultation
- After an appointment with an in-home care professional
- After a treatment or surgery
- After in-home medical equipment training
- After a patient has started a new course of medication
Follow-up email communications could include advice on booking a subsequent appointment, aftercare advice, or guidelines for taking medication. Again, as with appointment reminders, follow-up emails can be automated to streamline the process.
3. Personalized Treatment Plans
Tailoring treatment plans to fit a patient’s specific needs enhances treatment efficacy and reduces the likelihood of adverse effects. Secure email plays a crucial role in the development and distribution of treatment plans, which always include PHI, providing a channel by which healthcare providers can share sensitive patient data quickly and coordinate on any courses of action.
Email security measures, such as encryption, access control, and user authentication protect patient data from the malicious efforts of cybercriminals, while ensuring compliance with HIPAA’s Security Rule.
4. Care Coordination
Effective care coordination is essential for in-home care success where multiple healthcare professionals, such as nurses, therapists, and caregivers, must consistently collaborate to deliver high levels of patient care.
Offering critical functions such as treatment updates and emergency alerts, HIPAA-compliant email communications can ensure that all necessary parties remain in the loop about any situations regarding their shared patients. Additionally, integrating HIPAA-compliant email with a customer data platform (CDP) solution, electronic health record (EHR) systems, or any other system where PHI resides, allows in-home care providers to access and update patient records in real time, ensuring access to up-to-date information across the care team.
5. Proactive Patient Education
Educating patients through secure, personalized communications helps to enhance their competence in matters regarding their health, thereby increasing confidence in their ability to manage their healthcare journey more effectively, and resulting in greater engagement. Using PHI to segment patients by their condition or certain demographics (e.g., age, gender, lifestyle factors) and send them relevant educational materials is a powerful way for in-home care providers to offer additional value. This could include:
- Advice on managing a particular condition of injury, e.g., chronic disease management
- Informing patients and customers of events related to their present state of health, e.g., classes for expectant mothers, support groups for cancer patients, etc.
- Tips related to improving their health according to recent diagnoses and known lifestyle factors, e.g., smoking cessation strategies, dietary advice, etc.
Patient education is such an effective use of HIPAA-compliant email because it can be done frequently. Plus, it offers the additional benefits of helping to position the in-home care provider as an expert, increasing patient trust and boosting adherence to prescribed health advice.
6. Collecting Patient and Customer Feedback
Another simple, yet powerful use of secure email communication is to collect feedback and intelligence from patients, via integrated, secure email and forms, for review requests, surveys, and polls. By gaining insight into how your patients and customers feel about the quality of your in-home care products and services, you can pinpoint areas for improvement. As well as increasing customer satisfaction levels, this will also present opportunities to root out inefficiencies and cut costs in the process.
Additionally, asking for feedback helps increase patient trust, because you’ve displayed a commitment to improving your service and that you’re interested in the opinion of your patients and customers.
7. Health Alerts
HIPAA-compliant email is a helpful tool for making patients aware of situations or circumstances that could adversely affect their health. This could include alerts about virus outbreaks in their area or adverse weather events that could affect their in-home healthcare provision. To maximize value, these email alerts can be paired with advice to help patients through potential health emergencies, such as information on vaccine drives, activities to avoid during a period of rough weather, and support resources should they require more assistance.
Elevate Your In-Home Care Communications with LuxSci HIPAA-Compliant Email
LuxSci stands at the forefront of secure healthcare communications, offering HIPAA-compliant email, text, forms and marketing solutions for the security and compliance needs of in-home care providers. With over 25 years of experience, LuxSci provides secure high-volume email solutions, solutions for making Google Workspace and Microsoft 365 HIPAA-compliant, secure text messaging, and secure forms solutions that enable personalized, efficient, and effective patient engagement across a variety of channels.
Using LuxSci’s suite of secure communication tools, in-home care providers can streamline their operations, drive better, more personalized engagement, and improve health outcomes for the growing numbers of patients looking for healthcare services at home. Contact LuxSci today to learn more.